Santa Clarita resident Jessica Lewis grabbed her son Nathaniel’s hand as they walked out the doors of Children’s Hospital Los Angeles, a familiar path for them.
But on Friday, their journey changed — for the better. After more than 32 endoscopies, Nathaniel enjoyed an important “first.”
“This new procedure is a game-changer and it’s going to make it so much easier on everybody,” said Lewis. “We’re really pushing along. He has had his feeding tube for over two and a half years now. He just wants to be normal.”
“The even better thing is, I don’t have to get pushed out of here in a wheelchair,” said Nathaniel, smiling. “This one is a lot easier because I didn’t have to wake up early and have the IV and all that kind of stuff.”
Nathaniel was the first to receive this type of endoscopy procedure on the West Coast, a transgastric endoscopy.
Nathaniel had his first endoscopy when he was just 3 months old, his mother said. “He didn’t have any more until he was 5, and it’s been every two to four months since then.”
At the age of 6, he was diagnosed with Eosinophilic esophagitis, also known as EoE. This is a chronic allergic inflammatory disease of the esophagus, Jessica Lewis said. “It has actually eaten valleys into his esophagus, that are permanent, and when he’s flaring from his condition, it’s worse.”
Nathaniel also has celiacs disease, which affects his diet and immune system, and Ehlers–Danlos syndrome, which causes his joints to dislocate.
During the procedure, they pulled out his “G” tube and put a camera in his stoma to do the endoscopy, instead of going through his throat or nose.
“There’s no risk with anesthesia,” Jessica Lewis said. “There’s zero recovery time.”
Before this new procedure, every two months, Nathaniel basically had to spend more than a day in preparation, and would have to undergo anesthesia every time he had an endoscopy — a nonsurgical procedure used to inspect a person’s digestive tract.
A routine endoscopy begins with 12 hours without food and water prior to the procedure, said Dr. Vrinda Bhardwaj, Valencia resident, director of GI Endoscopy Services and assistant professor of Clinical Pediatrics at CHLA.
The morning after the fast, the patient is given sedation to sleep, before the doctors use a small, spaghetti noodle-like device with a camera attached to take biopsies, and get a good look at their food pipes, stomach and intestines.
During a routine endoscopy, Nathaniel would be put to sleep, and his mother would then leave the room.
“What they worry about is, ‘Whether my child is going to wake up or not,’” Bhardwaj said. “That component goes away with this.”
The second benefit to this new type of endoscopy is there’s no need for sedation.
“We are not exposing our children to opioid medications,” Bhardwaj said. “We know the huge epidemic it is.”
The third advantage is not having an IV, not having to starve for a period of time and not missing school, the last of which is very important to Nathaniel, his mother said.
Whereas the old procedure had about a two-hour recovery time, this new method has zero recovery time, and can be done in less than a half-hour.

“This is a program that has literally revolutionized the way we do endoscopies,” said Bhardwaj. “What we are doing here now is we are doing it while they are awake and we are having them see the virtual reality movies and games, which keep them distracted.”
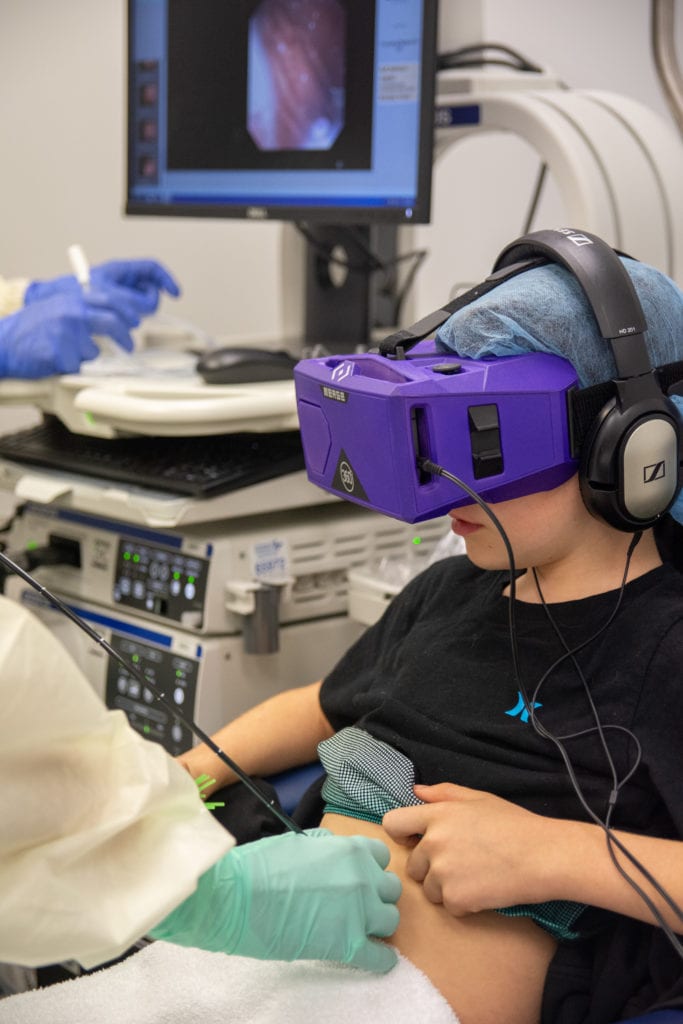
During Nathaniel’s procedure, he wore VR goggles, keeping him focused on one thing, the game he was playing.
“I was playing a game called ‘Bear Blast,’” he said. “You had a cannon and had to aim it to hit the bears with the cannon balls.”
During this new type of endoscopy, they have two mechanisms to do it, to go in through the nose or go into the food pipe and the stomach.
“We know endoscopies — for us the only thing that was different was doing it in an awake patient. The hardest thing there is getting them comfortable,” Bhardwaj said.
For children who have a G, or gastric tube, like Nathaniel, doctors can go into the patient’s stomach and then go look at their food pipe, Bhardwaj said. “With this, they can eat their breakfast in the morning, they meet us in two hours, we do the procedure, and it lasts seven to 15 minutes.”
The patients go home the same day, and they can eat and drink right away.
“The most important piece, which is different, is having family be a part of it,” Bhardwaj said.
“It’s really exciting, because I don’t have to leave him,” his mother said. “I can stay with him the whole time.”

He’s currently a fifth-grade student at Pinetree Elementary School in Canyon Country.
“He hates having any absences. He does not want to miss school at all,” Jessica Lewis said. “As soon as his endoscopies are done, we pack up and we drive all the way back out and he goes to school.”
Nathaniel loves being active, playing baseball, soccer, hockey and basketball.
“When he had the anesthesia, we couldn’t let him go do all those,” making this procedure very different than the 31 prior, his mother said.
“He had his normal breakfast, which is six slices of bacon, and he went back to sleep,” Jessica Lewis said. “He slept the whole way down here, and he wasn’t nervous about anything.”
The procedure is very patient-focused, Bhardwaj said. “It’s been a really long journey getting it together. It’s been very rewarding, and I wouldn’t have been able to do it without my team.”
The journey has been hard, his mother said. “Now, we can potentially introduce food a lot more often. We could introduce foods every couple weeks instead of waiting two months to reintroduce something. That speeds up our process a lot.”
Bison is the next food Nathaniel wants to try, he said.
“It will make it so he can get more of his life back,” Jessica Lewis said, “instead of being consumed by what he’s allowed to eat and what he’s not.”
-30-






